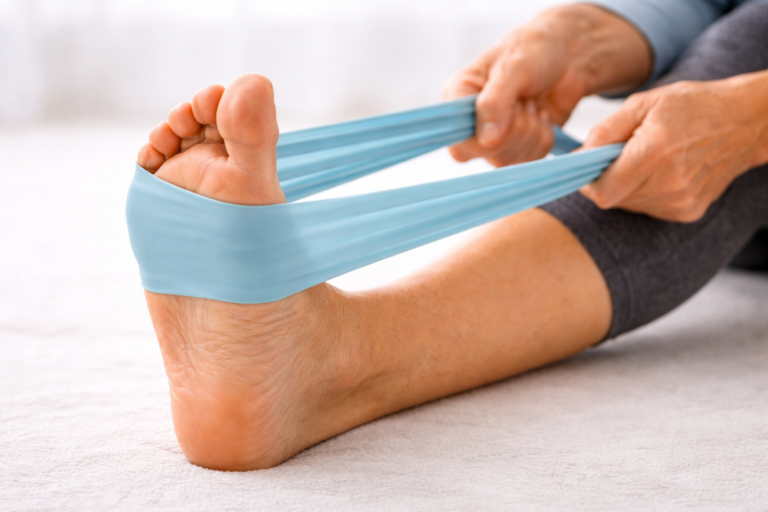
Does Walking Help Neuropathy? What the Research Actually Shows
Yes, and I have the study citations and four years of personal experience to back it up.
I was diagnosed with diabetic peripheral neuropathy in 2022. The burning in my feet was bad enough that I dreaded getting out of bed in the morning. My neurologist mentioned exercise almost as an afterthought. “Try walking,” she said. I went home and spent two hours looking for actual evidence that this would do anything.
What I found surprised me. Walking, regular, consistent, low-to-moderate intensity walking, is one of the most studied non-pharmacological interventions for peripheral neuropathy. The evidence is a lot stronger than most people realize.
Key Takeaways
- Multiple randomized controlled trials show aerobic exercise, including walking, significantly reduces neuropathy pain and improves nerve function.
- Walking improves intraepidermal nerve fiber density, meaning nerves can partially regrow with consistent exercise.
- 30–45 minutes of moderate-intensity walking, three to five times per week, is the most supported protocol in current research.
- Foot safety, proper shoes, surface choice, daily foot checks, is non-negotiable when you have neuropathy.
- If walking is too painful to start, pool walking and recumbent cycling are evidence-backed alternatives.
What the Research Says About Walking and Neuropathy
A 2017 randomized controlled trial published in Frontiers in Neuroscience assigned adults with diabetic peripheral neuropathy to either a supervised aerobic walking program or standard care. After 16 weeks, the walking group showed statistically significant reductions in pain scores, improved balance, and, most importantly, increased intraepidermal nerve fiber density (IENFD) on skin punch biopsy. That last finding matters: it means the nerves themselves showed measurable regrowth, not just symptom masking.

A 2021 meta-analysis in Diabetes Care pooled data from 20 trials and over 1,000 participants with diabetic neuropathy. Aerobic exercise, predominantly walking-based protocols, produced consistent improvements in neuropathic pain, vibration perception threshold, and nerve conduction velocity. Research from the NIH’s National Institute of Diabetes and Digestive and Kidney Diseases also notes that physical activity improves peripheral circulation and glycemic control, both directly relevant to neuropathy progression.
How Walking Helps: The Mechanisms
Improved Blood Flow to Peripheral Nerves
Nerves need a continuous oxygen supply. In peripheral neuropathy, microvascular damage reduces blood flow to the small vessels (vasa nervorum) that feed the nerves themselves. Aerobic exercise promotes angiogenesis, the growth of new capillaries, and improves endothelial function. Over time, this restores some of the oxygen delivery that damaged nerves depend on.
Nerve Fiber Regeneration
Multiple independent research groups have documented increases in IENFD following sustained aerobic exercise programs. Small nerve fibers, the ones responsible for temperature sensation and pain, appear capable of partial regrowth when blood supply improves and inflammatory markers decrease.
Pain Modulation via Central Sensitization
Chronic neuropathic pain involves a sensitized central nervous system that amplifies pain signals. Regular aerobic exercise has well-documented effects on central pain modulation: it increases endogenous opioid production, reduces inflammatory cytokines (particularly IL-6 and TNF-alpha), and helps recalibrate the brain’s pain processing systems.
Glycemic Control (for Diabetic Neuropathy)
For those of us with diabetic neuropathy specifically, exercise directly addresses a root cause. Skeletal muscle contraction improves insulin sensitivity and glucose uptake independent of insulin. A 45-minute walk can meaningfully reduce post-meal blood sugar spikes. Over months and years, better glycemic control slows the progression of nerve damage.
How Much Walking Is Needed?
- Frequency: 3–5 times per week
- Duration: 30–45 minutes per session (can be broken into 10–15 minute segments if needed)
- Intensity: Moderate, you should be able to hold a conversation but feel your breathing increase
- Progression: If sedentary, begin with 10–15 minutes at an easy pace and add 5 minutes per week
The Diabetes Care meta-analysis found that trials exceeding 150 minutes of activity per week produced larger effect sizes than shorter protocols. Consistency matters more than any single session, four weeks of regular walking produces measurable changes in nerve fiber density; eight to twelve weeks is where most trials start seeing significant pain reduction.
How to Walk Safely With Neuropathy
Footwear
Wear shoes specifically designed for diabetic feet if possible, wider toe boxes, extra depth, minimal internal seams that could cause blisters. If wearing standard athletic shoes, make sure they fit well, offer good cushioning, and have no areas of internal friction. Avoid bare feet or thin-soled shoes.
Surface
Flat, even surfaces are safest. Treadmills, paved paths, and indoor tracks are better choices than uneven trails or grass. Uneven terrain increases fall risk significantly when you have reduced sensation in your feet.
Daily Foot Checks
After every walk, inspect your feet, top, bottom, between the toes. Look for blisters, redness, cuts, or any areas of pressure. Because neuropathy reduces pain sensation, you may develop a blister or wound without feeling it. Catching problems early prevents serious complications.
What to Do If Walking Is Too Painful
Not everyone can start with a 30-minute walk. If standing and walking produce severe pain, there are well-supported alternatives.
Pool walking reduces your effective body weight by roughly 80%, eliminating most mechanical stress on painful feet. The resistance of water also provides a cardiovascular challenge.
Recumbent cycling removes weight from the feet entirely while still providing aerobic exercise and engaging the leg muscles that support peripheral circulation.
Seated leg exercises maintain circulation and muscle activity when even cycling is too much. For a complete list of options, see our guide to exercises for neuropathy in feet.
Mark’s Personal Walking Routine
I walk 40 minutes every morning, six days a week. I use diabetic-specific footwear. I walk on a paved trail near my neighborhood. I check my feet when I get home.
The first two months were hard. Around week ten, the burning in my feet was consistently less in the morning. By month four, my neurologist noted improvement in vibration perception on my left foot during a follow-up exam. I’m not cured. The neuropathy is still there. But it is measurably better than it was, and my last A1C was the best it has been in eight years. The walking is the only significant thing I changed.
For other approaches to combine with exercise, our article on natural ways to relieve neuropathy covers several options with evidence behind them.

Frequently Asked Questions
Can walking make neuropathy worse?
In most cases, no, but there’s an important nuance. Walking on damaged or blistered feet without realizing it can cause serious wounds. This is why daily foot checks and proper footwear are essential. The exercise itself does not damage nerves; neglected foot injuries do. Start gently, progress slowly, and check your feet every time.
What kind of shoes are best for walking with neuropathy?
Look for diabetic or therapeutic footwear with a wide toe box, extra depth, seamless interior lining, and firm but cushioned sole. Your podiatrist or certified diabetes educator can provide a specific recommendation based on your foot shape and gait.
Is swimming better than walking for neuropathy?
Swimming offers comparable cardiovascular benefits with less mechanical stress. For people with severe pain who cannot tolerate land-based walking, water-based exercise is an excellent starting point. For most people, walking has the practical advantage of requiring no pool access. Ideally, use both.
How long until walking helps neuropathy symptoms?
Based on clinical trials, most people begin noticing improvement in pain scores around 8–12 weeks of consistent exercise. Measurable changes in nerve fiber density have been documented at 16 weeks. Some people notice earlier improvements in mood, sleep, and overall fatigue.
Should I walk if I am having a neuropathy flare?
A mild flare does not necessarily mean you should skip your walk, but you should reduce intensity and duration. A gentle 10–15 minute walk at an easy pace is generally safer than complete rest. A severe flare, especially with new or unusual symptoms, warrants a call to your doctor before continuing.
Conclusion
The evidence is clear: regular walking meaningfully reduces neuropathy pain, supports nerve fiber regrowth, and improves the underlying factors, circulation, glycemic control, inflammation, that drive neuropathy progression. It’s not a cure, and it takes months of consistency to produce noticeable results. But of all the interventions I’ve tried and researched, it’s the one with the broadest and most reliable evidence base.
Start where you are. If 10 minutes is all you can manage, start there. Use the right shoes, check your feet, and be patient with the timeline. For further reading, explore our guides on exercises for neuropathy in feet and natural ways to relieve neuropathy.
Walking helps, but it works best as part of a broader approach that also addresses what’s damaging the nerves internally. Here’s what I’ve added to my own routine.
What I Use for Nerve Support
After 2 years testing supplements for peripheral neuropathy, Arialief is the formula that addresses the most mechanisms at once: antioxidant protection (ALA + B vitamins), anti-inflammatory support, and nerve regeneration cofactors.
Read My Full Arialief Review →Affiliate disclosure: I receive a commission if you purchase. This doesn’t affect my assessment.
Medical Disclaimer: The information in this article is for educational purposes only and does not constitute medical advice. Mark Whitfield is not a medical professional. Always consult your physician, neurologist, or certified diabetes educator before starting a new exercise program, particularly if you have peripheral neuropathy, cardiovascular disease, or other conditions that affect your ability to exercise safely.