Exercises for Neuropathy in Feet: 8 Gentle Moves That Actually Help
When my doctor told me I had diabetic peripheral neuropathy, my first instinct was to stop moving. My feet already felt like they were wrapped in wet cotton — burning, tingling, occasionally numb. The last thing I wanted to do was push them further.
That was three years ago. I was 51, a recently retired science teacher, and scared. What I know now is that staying still was the worst thing I could have done. Carefully chosen movement became one of the most effective tools I found for managing my symptoms. Not a cure. But a real, measurable difference in how my feet feel and how steadily I walk.
Key Takeaways
- Exercise improves blood flow to damaged nerves, which can slow progression and reduce pain.
- Balance and stability exercises are especially important — neuropathy increases fall risk.
- Start slow. Shorter sessions done consistently beat long sessions done sporadically.
- Always check your feet before and after exercise for wounds or irritation.
- Talk to your doctor before starting any new exercise program with neuropathy.
Why Exercise Helps Neuropathy (The Science)
Blood flow to nerves. Peripheral nerves depend on small blood vessels called vasa nervorum to deliver oxygen and nutrients. Exercise — even moderate walking — improves microvascular circulation, helping restore some of that supply to starved nerve tissue.


Nerve conduction. A 2016 study in the Journal of Diabetes and Its Complications found that a structured exercise program improved nerve conduction velocity in patients with diabetic peripheral neuropathy.
Pain perception. Exercise triggers endorphin release and increases brain-derived neurotrophic factor (BDNF), a protein that supports nerve health and pain modulation.
Balance and proprioception. Neuropathy disrupts proprioception — your body’s ability to sense where your feet are in space. Targeted balance exercises can partially compensate for this by training other sensory systems.
Safety Notes Before You Start
- Check with your doctor first — especially if you have open foot wounds, severe balance problems, cardiovascular disease, or poorly controlled blood sugar.
- Inspect your feet before and after every session. Neuropathy reduces your ability to feel cuts, blisters, and pressure sores. If you find a wound, do not exercise until it heals.
- Wear proper footwear — diabetic shoes or well-fitted athletic shoes with cushioned soles. Never exercise barefoot if you have sensory loss.
- Exercise in a safe environment. Clear the floor of rugs and cords. Have a chair or wall nearby for balance exercises.
- Stop if you feel sharp pain, unusual weakness, or chest pain.
The 8 Exercises for Neuropathy in Feet
1. Seated Leg Raises
Sit upright in a sturdy chair with both feet flat on the floor. Slowly straighten your right leg until parallel to the floor, hold 3–5 seconds, then lower slowly. Do 10 repetitions, then switch legs. Work up to 2–3 sets.
Why it helps: Activates the quadriceps and hip flexors, improving circulation through the entire lower limb. Modification: If straightening fully is painful, extend only to a comfortable angle.
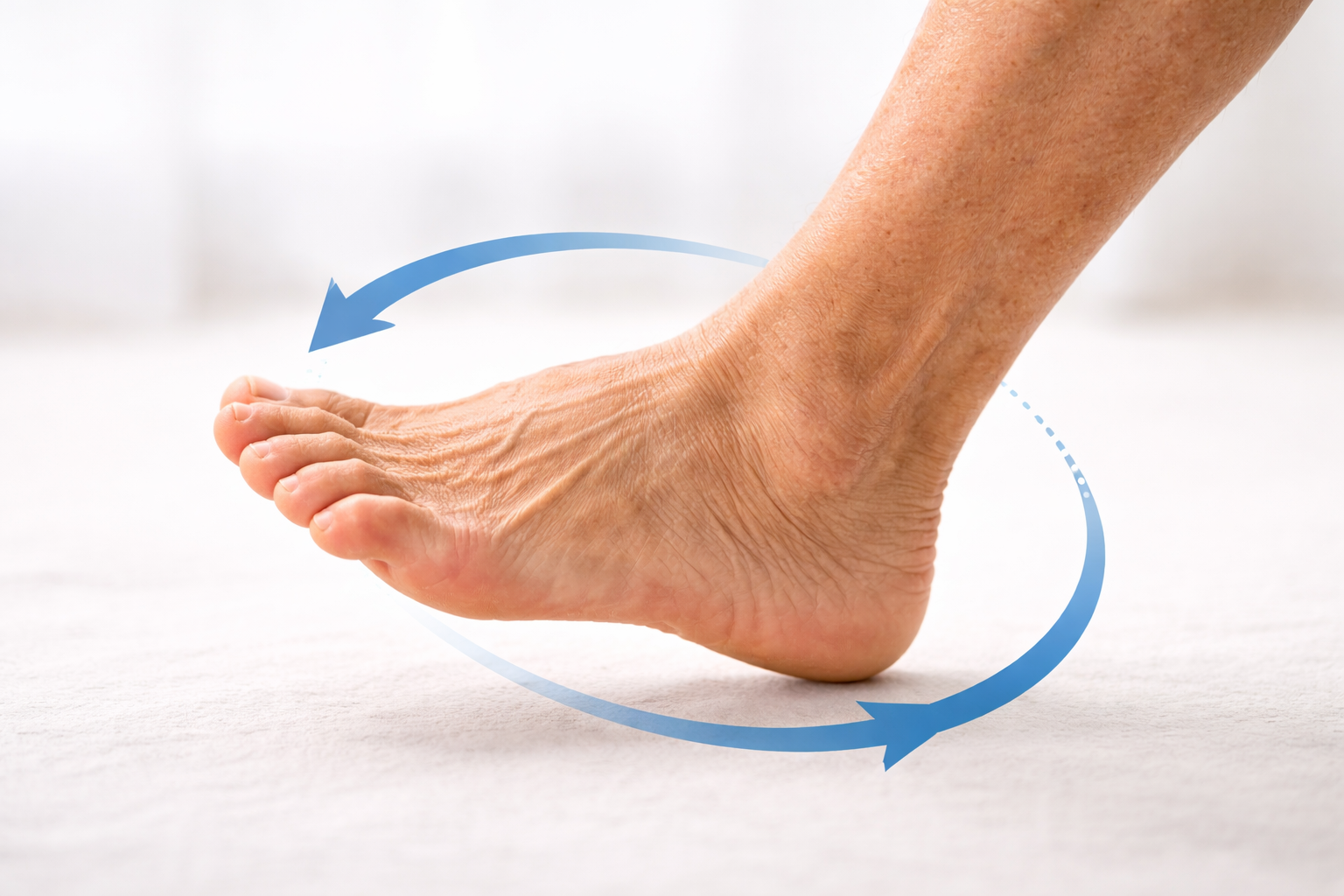
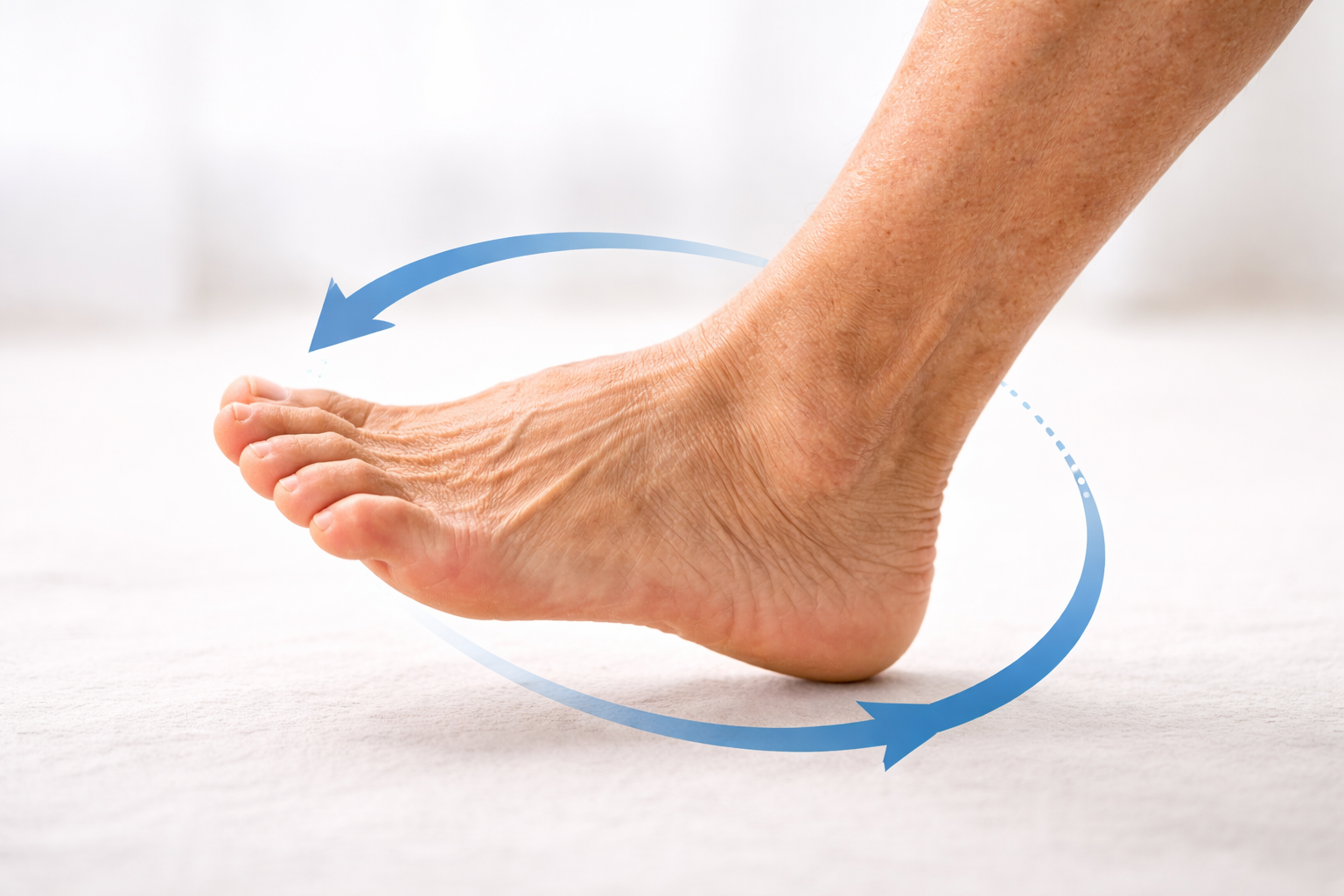
2. Ankle Rotations
Sit in a chair and lift one foot a few inches off the floor. Slowly rotate the ankle clockwise — 10 full circles — then reverse for 10 counterclockwise circles. Switch feet. Repeat 2–3 times per foot.
Why it helps: Mobilizes the joint, pumps synovial fluid, and stimulates blood flow to the lower foot and toes — an area that often has the worst circulation in neuropathy. Modification: Rest your heel on the floor and rotate from there if lifting is difficult.
3. Toe Curls With a Towel
Lay a small hand towel flat on the floor. Place your foot on the towel. Curl your toes to scrunch and pull the towel toward you. Release and spread it back out. Repeat 10–15 times per foot.
Why it helps: Targets the intrinsic muscles of the foot that control toe movement and arch stability. Neuropathy often weakens these muscles, contributing to foot drop and instability. Modification: Use a textured mat to add tactile input if you have reduced sensation.
4. Calf Raises (Seated)
Sit in a chair with feet flat on the floor. Slowly raise both heels as high as comfortable, coming onto the balls of your feet. Hold 2–3 seconds at the top. Lower slowly (3-count). Do 15 repetitions, 2–3 sets.
Why it helps: The calf muscles act as a venous pump — their contractions push blood back up toward the heart. Weak calves mean poor venous return, which worsens nerve ischemia. Modification: When ready, progress to standing calf raises while holding a chair.
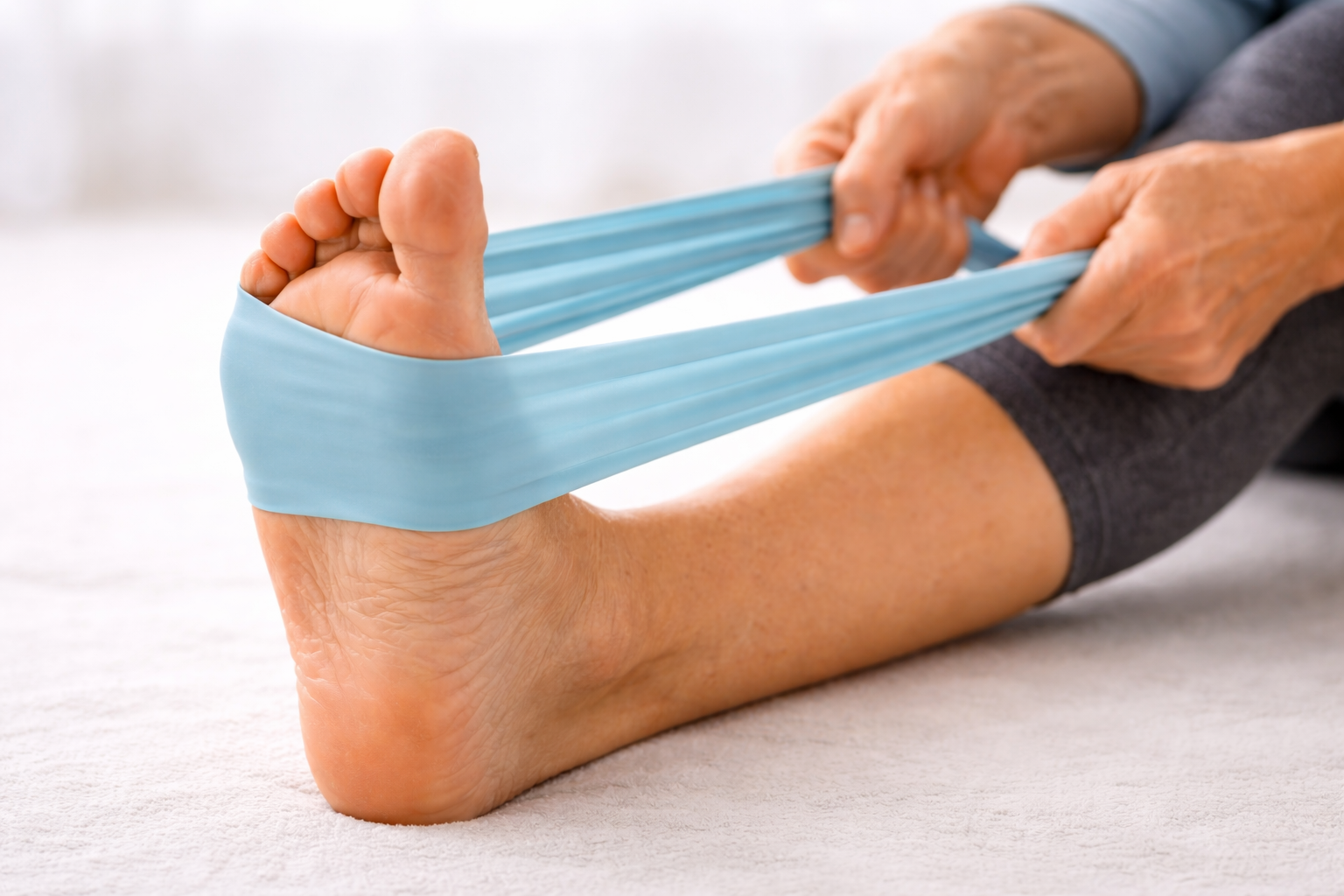
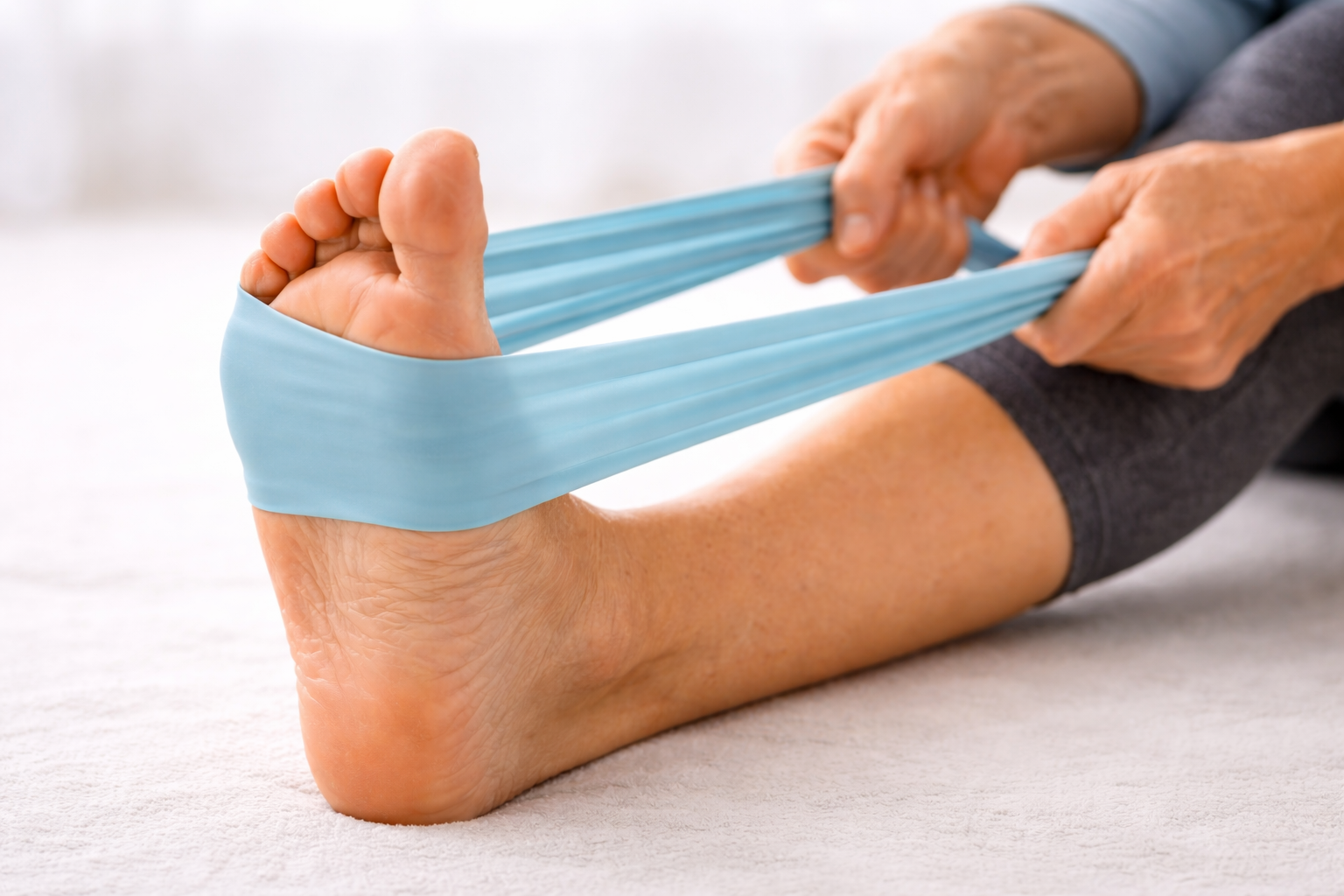
5. Resistance Band Foot Flexion
Loop a light resistance band around the ball of one foot, holding both ends. Slowly flex your foot toward you (dorsiflexion) against the band, hold 2 seconds, then slowly point the foot away. Do 12–15 repetitions per foot, 2 sets.
Why it helps: Weak dorsiflexors are a major contributor to foot drop, a common and dangerous consequence of peripheral neuropathy. Modification: Use the lightest band available, or a folded bedsheet or long scarf. Gentle resistance, not heavy load.
6. Balance Standing (Eyes Open to Eyes Closed)
Stand near a wall or chair. Begin standing on both feet, eyes open, for 30 seconds. Progress to one foot for 15–30 seconds. When comfortable, try the same with eyes closed (one foot at a time, near the wall). Build up to 3 repetitions per side.
Why it helps: Balance training forces your nervous system to compensate using vision and vestibular input — multiple studies show it significantly reduces fall risk in people with peripheral neuropathy. Modification: Never close your eyes unless someone is present or you have a solid wall within arm’s reach.
7. Walking (Gentle, Flat Surface, Proper Footwear)
Start with 10 minutes on a flat, unobstructed surface at a comfortable pace. Add 2–5 minutes per week as tolerated. Work toward 30 minutes most days of the week.
Why it helps: A landmark 2006 study in Diabetes Care found that regular walking reduced neuropathic pain and improved quality of life in people with type 2 diabetes and neuropathy. It improves circulation, stimulates nerve tissue, builds lower-limb strength, and helps regulate blood sugar. Modification: A treadmill with handrails is an excellent alternative if outdoor walking is unsafe.
8. Tai Chi or Gentle Yoga
Find a beginner-level tai chi or chair yoga class focused on “balance and stability” or “fall prevention.” A 2012 randomized controlled trial in the New England Journal of Medicine found that tai chi outperformed a structured exercise program for improving balance and reducing falls in older adults.
Modification: Chair yoga is an excellent entry point if standing balance is unreliable. Even 15 minutes two to three times per week shows measurable improvement.
How Often to Exercise With Neuropathy
- Aerobic activity (walking): 5 days per week, 20–30 minutes per session. Start at 10 minutes and build gradually.
- Strengthening exercises: 3 days per week, with at least one rest day between sessions.
- Balance training: Daily, 5–10 minutes. Low-intensity enough to do every day.
- Tai chi or yoga: 2–3 times per week, 20–30 minutes per session.
Consistency matters more than any single session. Three 20-minute sessions per week done every week beat six-day programs that collapse after two weeks. When starting out, even 10 minutes of walking and 5 minutes of seated exercises is fine. Build from there. If you’re experiencing neuropathy symptoms that are new or worsening, speak with your doctor before increasing exercise intensity.
Signs You Are Overdoing It
- Increased pain lasting more than an hour after exercise
- New blisters, redness, or pressure sores on your feet
- Swelling in the feet or ankles that doesn’t resolve with elevation
- Significant increase in tingling or burning for more than a day after a session
- Falls or near-falls — your balance work should be progressing, not getting worse
- Fatigue that interferes with daily function — exercise should energize you over time, not exhaust you


Frequently Asked Questions
Can exercise actually reverse neuropathy?
In most cases, no — particularly if nerve damage is already moderate to severe. However, exercise has been shown to slow progression, improve nerve conduction in some patients, and significantly reduce pain and balance problems. Think of it as management, not reversal.
What if my feet are too numb to feel what I’m doing?
That is common, especially early in the process. Focus on exercises where the movement itself is controlled and safe regardless of sensation — seated exercises, supported balance work, and resistance band movements are good starting points. The goal is not to feel the sensation; it’s to maintain the muscle and vascular health that supports your nerves.
Is swimming or cycling better than walking for neuropathy?
They are all valid options. Swimming removes the impact and balance risk that walking involves — excellent for people with severe balance issues. Cycling is similarly low-impact. Walking has the most evidence specifically for diabetic neuropathy, but the best exercise is the one you will actually do consistently.
How long before I notice improvement?
Most people report some improvement in pain levels and balance within 6–8 weeks of consistent exercise. Significant functional improvement typically takes 3–6 months. There will be days that feel like regression — that is normal and not a signal to stop.
Should I exercise if I have a foot wound?
No. A foot wound in someone with neuropathy is a medical issue requiring prompt attention. Rest until the wound is healed and cleared by your doctor. Upper body exercise may be fine, but get specific guidance from your care team.
Conclusion
Three years after my diagnosis, I walk 25 minutes most mornings. My balance is significantly better than it was at my worst. The burning in my feet is still there — I am not going to pretend it disappeared — but it is manageable. I sleep better. I feel more in control.
Start with one or two exercises from this list. Do them seated. Do them for 10 minutes. Then do it again tomorrow. For more on managing this condition, read our guide to natural ways to relieve neuropathy pain. And if you’re still getting your bearings on the diagnosis, our overview of peripheral neuropathy is a good starting point. You do not have to stay still.
Medical Disclaimer: The content in this article is written by Mark Whitfield, a patient living with diabetic peripheral neuropathy, based on personal experience and published research. It is for informational purposes only and does not constitute medical advice. Always consult your physician, podiatrist, or licensed physical therapist before beginning any new exercise program. Individual results vary.




